Just Group said that the latest Office for National Statistics data presents a mixed picture of how the country’s health is recovering from the coronavirus (COVID-19) pandemic.
Between 2022-24, life expectancy at birth rose across all wealth levels (deprivation deciles) compared to 2019-2021 for both men and women, although it was still lower in the most deprived decile compared to the period immediately before the pandemic (2017-19).
But the ONS estimate that healthy life expectancy (HLE) decreased across all wealth levels compared to 2019-21 with the greatest decreases found in the more deprived areas. HLE decreased by 3.2 years for females and 2.2 years for males in the most deprived decile, but also by 1.8 years for females and 1.2 years for males in the least deprived (wealthiest) decile.
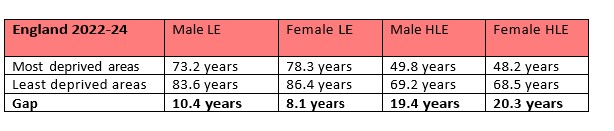
There is a significant equality gap between deprivation deciles. Life expectancy at birth for males was 10.4 years lower in the most deprived areas compared to the least deprived and 8.1 years for women. Similarly, the divide in healthy life expectancy between the most and least deprived areas was 19.4 years and 20.3 years for men and women, respectively.
David Cooper, director at retirement specialist Just Group, said the figures show a widening inequality, not just in how long people live, but how long they live in good health: “A woman in the least deprived area of England can expect, on average, to live around eight years longer than her counterpart in the most deprived areas; for men that gap is 10 years,” he commented.
“Even more striking is the discrepancy in healthy life expectancy – both men and women in the least deprived areas of England can expect to enjoy, on average, around twenty years more in healthy life expectancy than their counterparts in the most deprived areas.
“Inequality represents a huge challenge because those from poorer areas are more likely to be forced out of the workforce earlier due to ill health, while also having fewer financial resources to fall back on before reaching State Pension age.
“It sharpens the focus on the adequacy and flexibility of retirement income solutions. People may need access to their pension savings earlier, or in a more tailored way, to bridge gaps in income and support changing health needs over time. At the same time, the growing period spent in later life with complex health conditions reinforces the importance of planning for care, which remains one of the most significant – and often underestimated – financial risks in retirement.”
The ONS figures are useful for policymakers trying to understand current health trends across the whole population because they are based on historic mortality and assume no impact from future medical breakthroughs or lifestyle improvements. A 65-year-old living in the same areas would be expected to have a significantly higher age of death because their life expectancy depends only on death rates beyond their age, whereas survival from birth is based on death rates at every age.
|

